America’s next big health revolution is arriving through wearables and AI—but the same data that could help you live to 100 could also invite a new era of surveillance medicine if Washington ever gets its hands on it.
Quick Take
- CES 2026 featured nearly 100 longevity exhibitors, signaling that “healthspan” tech is moving fast from niche biohacking into everyday consumer products.
- New tools aim to shift healthcare from reactive treatment to proactive monitoring, using daily biometrics, AI analysis, and at-home testing.
- Standout categories include sleep and recovery wearables, mobility-assist devices, AI heart-disease screening, and AI companions for seniors.
- GLP-1 drugs like Ozempic are being discussed for broader longevity benefits, but long-term outcomes and appropriate use still require careful clinical grounding.
CES 2026 Put Longevity Tech Into the Mainstream
CES 2026 did not treat longevity as a sci-fi sideshow. Reporting on the event described a surge of “longevity” exhibitors—nearly 100—showing gadgets and services designed to measure, predict, and improve the aging process. The emphasis was not on secret labs for billionaires, but on consumer-accessible devices that collect health signals daily. That scale matters: once technology is marketed as routine wellness, it spreads quickly into workplaces, insurers, and clinical workflows.
Several showcased tools aim at practical, day-to-day problems older Americans actually face. Sleep and recovery tracking devices such as smart rings focus on patterns that affect energy, metabolism, and resilience. Mobility-support concepts like an exoskeleton target stability and independence—an area where dignity and self-reliance matter more than buzzwords. A key throughline is continuous measurement: instead of an annual physical, the pitch is always-on feedback that nudges behavior and flags risk earlier.
From “Sick Care” to Early Warnings: AI Meets Everyday Biometrics
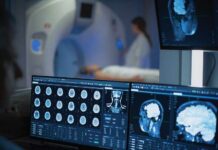
The research highlights a clear theme: healthcare tech is moving from reactive intervention to proactive detection. Products and services discussed include AI-assisted heart-disease tools that analyze imaging for plaque and consumer devices meant to track biomarkers at home. Advocates describe “ambient longevity,” where ordinary lifestyle data—sleep, movement, heart signals, and more—feeds AI systems that offer personalized coaching. Done responsibly, this could help families catch problems earlier and reduce preventable decline.
That promise comes with a straightforward concern: the more intimate the data, the higher the stakes. The research focuses on consumer empowerment, but it also signals how easily “personalized health” can become institutional pressure if tied to employers, insurers, or government programs. Americans who lived through years of bureaucratic overreach understand the risk: a tool sold as optional can become a de facto requirement. The technology itself is not the villain; the danger is who controls it and what strings get attached.
Drugs, Devices, and the Rush to “Healthspan” Markets
Beyond devices, the research notes continued attention to drug repurposing and longevity-linked outcomes. GLP-1 medications such as Ozempic and related drugs are discussed in the context of reduced hospitalization and mortality signals cited by an aging researcher, pointing to a broader “healthspan” narrative rather than simple weight loss. At the same time, the research acknowledges uncertainty: dramatic claims about maximum lifespan and long-term results remain debated, and hype can outrun evidence.
Investment and prestige also shape this space. Venture-backed efforts and high-profile tech figures are connected in the research to trials and ambitious projects, fueling a wider conversation about unequal access. The concern is not merely envy—it is whether the longevity economy becomes a two-tier system where affluent early adopters get premium screening and interventions while everyone else gets delayed care and higher costs. That tension will drive future policy fights over approvals, coverage, and data governance.
What This Means for Families, Freedom, and Policy in 2026
For older Americans and their families, the practical upside is easy to see: tools that support mobility, detect heart risk earlier, and reduce isolation could keep seniors independent longer. But in a country that values liberty, the policy question is just as important as the science. If longevity tech becomes a justification for centralized control—mandated monitoring, coerced “compliance,” or data-sharing schemes—then innovation could end up eroding personal autonomy instead of strengthening it.
Limited-government conservatives should watch how these tools are integrated into healthcare systems, insurance incentives, and federal health guidance. The research shows legitimate momentum toward preventative care, but it also shows a market racing ahead of long-term validation for some claims and a growing ecosystem hungry for data. The best path forward is transparency, voluntary adoption, strong privacy norms, and reforms that let patients—not bureaucracies—decide which technologies belong in their lives.
Sources:
How New Longevity Tech Could Help You Reach 100
Healthy, Holistic, and Happening Now: A Look at Longevity Trends for 2026
7 Cutting-Edge Therapies Revolutionizing Healthy Aging in 2026
Anti-aging and longevity startups to watch
Beyond aging clocks: AI longevity drug discovery
The Biological Secession: How Longevity Technology Will Create a New Species Divide