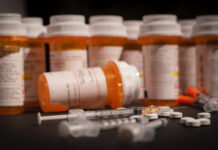
A cough lasting more than eight weeks despite standard treatment now has a formal diagnostic roadmap that could transform how millions of Americans get relief.
Quick Take
- Refractory chronic cough (RCC) is defined as persistent cough lasting over eight weeks that doesn’t respond to treatment for common causes like reflux, allergies, or lung disease.
- The American Broncho-Esophagological Association issued its first expert consensus statement in May 2026, establishing specific diagnostic criteria and treatment protocols for otolaryngologists and other specialists.
- Diagnosis requires documented adequate testing including chest imaging, pulmonary function tests, and empiric trials before a cough qualifies as truly refractory.
- Treatment options now include neuromodulators, superior laryngeal nerve blocks, and behavioral cough suppression techniques, moving beyond traditional approaches.
The Eight-Week Threshold That Changes Everything
Chronic cough affects roughly eight percent of Americans, but most cases resolve within weeks. The problem emerges when cough persists beyond eight weeks despite workup and treatment for reflux, sinus inflammation, and pulmonary disease [1]. This is where refractory chronic cough enters the clinical picture. The distinction matters because patients stuck in this category often bounce between specialists, accumulate unnecessary tests, and exhaust ineffective treatments before reaching someone who recognizes the condition’s true nature.
Defining Adequacy in Medical Workup
The consensus statement establishes what “adequate testing” actually means, a detail that has plagued the field for years. For pulmonary disease specifically, providers must document whether chest imaging has been completed, whether pulmonary function tests have been performed, and whether an empiric trial of inhaled steroids has been attempted [1]. Similar rigor applies to reflux and sinus disease assessment. This framework prevents premature labeling of cough as refractory when standard diagnostics remain incomplete, a common pitfall in specialty practice.
Treatment Beyond the Cough Syrup Aisle
The statement recommends three primary treatment pathways that represent a fundamental shift from symptomatic management. Neuromodulators target the underlying neural hypersensitivity driving persistent cough, while superior laryngeal nerve blocks interrupt the reflex arc directly [1]. Behavioral cough suppression techniques, often overlooked in conventional practice, address learned components of the cough reflex. This multi-modal approach acknowledges that refractory cough rarely yields to single interventions and requires personalized sequencing based on patient response and tolerance.
Why This Consensus Matters Now
The American Broncho-Esophagological Association’s decision to create a formal consensus process signals recognition that refractory chronic cough has become too prevalent and too complex for informal guidance [2]. This represents the first expert consensus statement from the association’s newly established clinical guidance process, expressly designed to translate evidence into actionable protocols. The timing reflects growing awareness that millions of patients remain trapped in diagnostic limbo, cycling through antibiotics, inhalers, and reflux medications that provide no relief.
The Specialty Convergence Problem
Pulmonologists, otolaryngologists, gastroenterologists, and allergists all claim legitimate expertise in chronic cough management, yet their guidelines sometimes diverge on priorities and thresholds [5]. The ABEA statement plants a flag for otolaryngology’s role in the diagnostic and therapeutic landscape, particularly regarding laryngeal mechanisms and nerve-based interventions. This specialty perspective complements rather than replaces pulmonology-centered approaches, but the distinction matters for patients seeking the right specialist first rather than cycling through multiple practitioners.
The Evidence Gap That Remains
Despite establishing clear diagnostic criteria and treatment recommendations, the consensus statement acknowledges that neuromodulator efficacy data and long-term outcomes for nerve blocks remain incomplete [1]. Established guidelines from other organizations rate some neuromodulators like morphine and gabapentin as conditional or low-evidence recommendations, with response rates around fifty percent and significant side effect profiles [7][8]. The ABEA statement moves forward with these tools anyway, reflecting clinical reality: patients desperate for relief often benefit from structured trials of options that lack perfect evidence but show promise in practice.
What Patients Should Expect
If you’ve had a cough for more than eight weeks and standard treatments haven’t worked, this consensus statement means your doctor now has a formal protocol to follow. Expect systematic evaluation of your lungs, sinuses, and reflux status before any label of “refractory” applies. If you qualify, treatment discussions should include neuromodulators with clear expectations about trial duration, behavioral techniques that require active participation, and potentially nerve blocks if other options fail. The framework replaces guesswork with structure, though individual outcomes remain unpredictable.
Sources:
[1] YouTube – Consensus Statement on the Diagnosis and Treatment of Refractory …
[2] Web – [PDF] American Broncho-Esophagological Association
[5] Web – WAO – ARIA consensus on chronic cough: Executive summary – PMC
[7] Web – ERS guidelines on the diagnosis and treatment of chronic …
[8] Web – Management of chronic refractory cough in adults – PMC