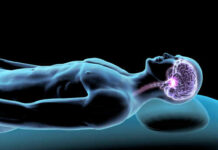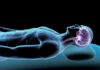
Your brain might be working against you every time you stand up, and scientists have pinpointed the exact group of cells responsible for betraying your balance as you age.
Story Snapshot
- Unipolar Brush Cells in the cerebellum become critical for balance maintenance in older brains but lose effectiveness with age
- Experiments on mice showed disrupting these cells devastated balance in older animals while young mice adapted easily
- The brain’s cortex overcompensates in aging, creating excessive muscle stiffness that actually worsens recovery from stumbles
- This cellular sabotage explains why older adults struggle more with conflicting sensory signals than simple balance tests
- Discovery shifts focus from general vestibular decline to precise neural targets for preventing falls
The Cellular Culprits Behind Your Unsteady Gait
Researchers targeting ataxia disorders discovered Unipolar Brush Cells lurking in the cerebellum, acting as unexpected gatekeepers of age-related stability. The Kizeev research team disabled these specialized neurons in both young and older mice using advanced techniques. Young mice at seven weeks old barely noticed the disruption, compensating through alternative neural pathways. Six-month-old mice, however, suffered dramatic balance failures. The cells that should protect older brains from wobbling instead become liabilities, their compensatory functions eroding precisely when needed most. This cellular betrayal represents a fundamental shift in understanding balance disorders, moving beyond vague “aging effects” to identified neural weaknesses.
When Your Brain Tries Too Hard and Fails Anyway
Lena Ting’s research team uncovered a cruel irony in aging brains: they work harder but perform worse. Measuring cortical responses during balance perturbations, scientists found older adults and Parkinson’s patients generate excessive brain activity for minor stumbles. This neural overdrive triggers what Ting calls “co-activation stiffening,” where opposing muscle groups contract simultaneously. Young people deploy efficient two-wave muscle responses, the brainstem handling initial corrections while cortex reserves intervene only when necessary. Aging brains flood the system with cortical signals, creating rigid muscles that cannot adapt. Ting notes balance recovery takes more energy in older adults, yet more brain activity correlates with less robust recovery, a counterintuitive relationship that defies common assumptions.
The Sensory Conflict Your Aging Brain Cannot Resolve
Sensory Organization Tests revealed where aging brains truly falter. Older adults performed worst on SOT-6, which provides deliberately inaccurate visual and proprioceptive cues requiring central integration to ignore false signals. They handled SOT-5, eliminating visual input entirely, with relatively less difficulty. This pattern exposes central processing failures rather than simple sensory loss. The vestibular system loses twenty to forty percent of hair cells after age seventy, and the vestibulo-ocular reflex declines over five to ten years in healthy adults. Yet longitudinal studies show VOR decline precedes balance problems by years, suggesting peripheral degeneration alone does not explain unsteadiness. Roll-tilt threshold sensitivity mediates forty-six percent of the age-balance relationship, underscoring how central interpretation of motion cues deteriorates independent of sensor quality.
Why Young Brains Bounce Back and Old Brains Do Not
The flexibility advantage of youth operates at the cellular level. When researchers impaired UBCs in young mice, alternative cerebellar pathways assumed control within the experimental timeframe. Older mice demonstrated no such plasticity. This mirrors human data showing younger individuals reweight sensory inputs dynamically, shifting reliance between vision, proprioception, and vestibular signals as conditions demand. Aging reduces this reweighting capacity, leaving older adults trapped with maladaptive strategies. Brain atrophy and white matter lesions compound the problem, identified in 1990s prospective studies linking structural degeneration to falls. The National Institute on Aging now recommends central processing studies over peripheral vestibular research, recognizing compensation mechanisms matter more than isolated sensory decline.
George McInerney finds this interesting 👍 Why your brain may be sabotaging your balance as you age https://t.co/d3SF9LW3uV
— George McInerney (@gmcinerney) March 25, 2026
The multifactorial nature of disequilibrium emerged as a clinical term in the 1980s, describing dizziness and unsteady gait without single identifiable causes. Stanford Health Care now treats it as a syndrome involving vestibular nuclei, brainstem, cerebellum, cortex, and basal ganglia interactions disrupted by medications and pathology. Falls cost healthcare systems billions annually while causing social isolation through fear of falling. Families shoulder injury burdens as caregivers. Yet the UBC discovery offers hope for targeted interventions, shifting from broad balance training to cell-specific therapies that could preserve or restore the compensatory mechanisms aging steals.
Sources:
Aging and Parkinson’s Balance Brain Research – Neuroscience News
Age-Related Balance Decline and Sensory Organization – Frontiers in Neurology
Vestibular Function and Aging Research – PMC National Institutes of Health
The Surprising Reason Balance Gets Worse With Age and Parkinson’s – SciTechDaily
Keeping Your Balance as You Age – Dartmouth Health
Disequilibrium and Brain Atrophy Study – Neurology Journal
Disequilibrium of Aging – Stanford Health Care
Balance and Gait Disorders in the Aged Population – Dovepress